Non-tuberculous Mycobacteria (NTM)
Overview
Non-tuberculous mycobacteria (NTM) are bacteria belonging to the same family as those that cause tuberculosis. Unlike tuberculosis, which spreads from person to person, NTM infections come from the environment. NTM are found worldwide in soil, dust and contaminated water, including tap water and hot tubs. Patients can acquire infection through inhalation or by direct inoculation through the skin.
What Diseases Can NTM Cause?
- Lung infection
- Lymphadenitis
- Infection of the skin and soft tissue
- Disseminated disease (mainly in severely immunocompromised patients)
- Common NTM Species Causing Lung Infection in Hong Kong
- Mycobacterium kansasii
- Mycobacterium avium complex
- Mycobacterium abscessus
Causes/ risk factors
Most healthy people exposed to NTM do not get infected. Patients with chronic lung diseases such as bronchiectasis and chronic obstructive pulmonary disease (COPD), or those with weakened immunity, are more vulnerable to NTM infection.
Diagnosis
The diagnosis of NTM lung infection requires a combination of clinical, microbiological and radiological evidence.
- Symptoms
- Patients can have chronic cough, sputum, fatigue and weight loss.
- Bacterial culture
- Sputum samples are sent for smear and culture. Doctors may perform bronchoscopy to collect airway specimens for selected patients.
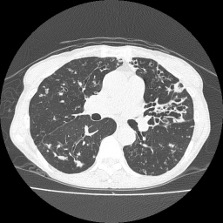
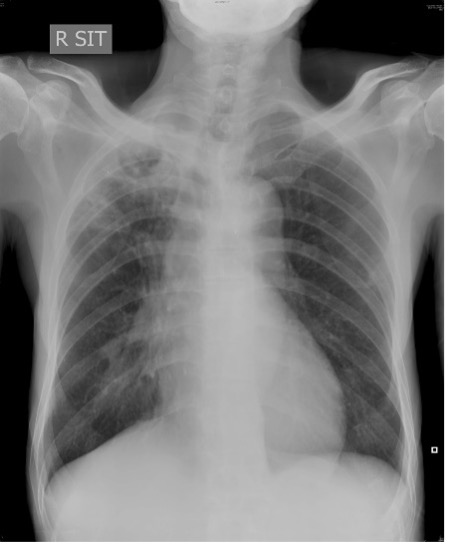
- Chest X-ray and CT thorax
- Common findings of NTM lung infection include bronchiectasis with lung nodules and cavities.
Treatment and Management
Standard treatment usually involves taking three to four antibiotics simultaneously for more than one year. Some infections, such as Mycobacterium abscessus, may require a combination of oral, injectable and nebulised antibiotics. Besides antibiotics, some patients with localised NTM lung infection may undergo surgery. Different NTM species have different treatment outcomes. Treatment adherence is important. Regular follow-up appointments, sputum tests and lung imaging can help monitor treatment progress.
Common Side Effects of Treatment
All medications can cause allergic reactions, e.g. itchy skin, urticaria, facial swelling and breathlessness.
- Azithromycin/ Clarithromycin
- Nausea, vomiting, diarrhoea
- Arrhythmia
- Liver injury, symptoms include nausea, vomiting, jaundice
- Tinnitus, hearing loss
- Ethambutol
- Blurring of vision
- Nausea, vomiting
- Rifampicin
- Nausea, vomiting, appetite loss
- Flu-like symptoms
- Liver injury, symptoms include nausea, vomiting, jaundice
- Blood disorders, symptoms include bruises and petechiae
- Orange discolouration of body fluids, e.g. urine, stool and tears
- Amikacin
- Tinnitus, hearing loss
- Kidney injury, symptoms include reduced urine and haematuria
- (Nebulised amikacin) Bronchospasm, hoarseness of voice, sore throat
Last updated: March 2026

