Interstitial Lung Disease (ILD)
Overview
Interstitial lung disease (ILD) refers to a group of lung disorders that affect the lung tissue (interstitium) around the air sacs (alveoli). In many forms of ILD, the lung tissue becomes inflamed and may gradually develop scarring (fibrosis). This can make the lungs stiffer and reduce the ability of oxygen to pass from the lungs into the bloodstream, leading to breathlessness.
Examples of ILDs:
- Idiopathic pulmonary fibrosis (IPF)
- Connective tissue disease – associated ILD (e.g. Rheumatoid arthritis, systemic sclerosis)
- Hypersensitivity pneumonitis
- Pneumoconiosis (e.g. silicosis or coal worker’s pneumoconiosis)

Common Symptoms
- Shortness of breath, especially during physical activity
- Persistent dry cough
- Reduced exercise tolerance or getting tired easily
- Fatigue
- Unintentional weight loss
- Chest tightness
Causes and risk factors
- Idiopathic causes (no identifiable cause) – for example idiopathic pulmonary fibrosis
- Autoimmune or connective tissue diseases such as rheumatoid arthritis or systemic sclerosis
- Exposure to environmental or occupational substances (e.g. silica, coal dust, mould, birds)
- Certain medications
- Infections (less commonly)
Diagnosis
- Medical history and physical examination
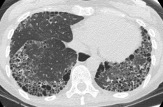
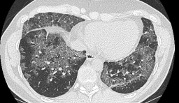
- Chest imaging such as chest X-ray or high-resolution CT scan
- Lung function tests
- Blood tests to look for autoimmune diseases
- In some cases, bronchoscopy or lung biopsy may be needed
Treatment and Management
- Treating the underlying cause when identified
- Anti-fibrotic medications for certain types of ILD
- Medications to reduce inflammation in selected cases
- Oxygen therapy for patients with low oxygen levels
- Pulmonary rehabilitation to improve exercise tolerance
- In advanced cases, lung transplantation may be considered
Living with ILD
- Attend regular medical follow-up
- Avoid smoking and harmful environmental exposures
- Maintain physical activity within your ability
- Receive recommended vaccinations such as influenza and pneumococcal vaccines
- Seek medical advice if symptoms worsen
Last updated: March 2026

