Sleep Apnea
Overview
We spend about one-third of our lives asleep. Quality sleep allows us to recharge after a busy day and face new challenges. However, many people suffer from sleep problems that affect their daytime energy, work performance, and even their long-term health. One common cause of these issues is Sleep Apnea.
What is Sleep Apnea?
Sleep apnea is a common sleep disorder. People with this condition experience repeated episodes of shallow breathing or stopped breathing during sleep. This leads to a drop in oxygen levels, disrupts sleep quality, and causes frequent awakenings throughout the night.
Many people mistakenly believe sleep apnea is “just snoring.” In reality, if left untreated, it can lead to a range of serious health problems, including high blood pressure, diabetes, heart rhythm problem, and cardiovascular disease.
Furthermore, the excessive daytime sleepiness and difficulty concentrating caused by sleep apnea can be dangerous. If a patient drives or operates machinery, it significantly increases the risk of traffic or industrial accidents, potentially causing serious injury or death.
Types of Sleep Apnea
Sleep apnea is classified into three main types: Obstructive, Central, and Mixed. Obstructive sleep apnea is the most common form.
- Obstructive Sleep Apnea (OSA)
This occurs when the muscles in the throat relax during sleep. This relaxation reduces support for the soft tissues in the airway (like the soft palate and uvula), causing them to collapse. When air passes through this narrowed or collapsed airway, it causes the tissues to vibrate, which creates the sound of snoring. If the airway becomes completely blocked, airflow stops, leading to a temporary pause in breathing. Causes of airway narrowing can include a deviated nasal septum, enlarged tonsils, or the tongue blocking the throat. - Central Sleep Apnea (CSA)
This type occurs when the brain fails to send the correct signals to the muscles that control breathing. This disrupts the normal rhythm of breathing. Causes may be related to brain conditions such as a previous stroke or head injury, heart disease, or the use of certain medications. - Mixed Sleep Apnea
This is a combination of both obstructive and central sleep apnea occurring in the same individual.
Common Symptoms
Nighttime Symptoms:
- Loud snoring, which may have intermittent pauses.
- A bed partner or family member observes periods where breathing stops during sleep.
- Waking up suddenly with a sensation of gasping or choking.
- Frequent need to urinate during the night (nocturia).
Daytime Symptoms:
- Waking up with a headache.
- Still feeling tired and unrefreshed after a full night’s sleep.
- Excessive daytime sleepiness, such as falling asleep easily at work, while watching TV, or even driving.
- Slow reaction times, irritability, and memory problems.
- Decreased libido (sex drive).
Causes/ Risk Factors
Several factors can increase your risk of developing sleep apnea:
- Age: Over 50 years old.
- Gender: More common in men.
- Lifestyle: Smoking and heavy alcohol use.
- Medications: Use of sleeping pills or sedatives.
- Weight: Obesity is a major risk factor.
- Medical Conditions: Underactive thyroid (hypothyroidism), high blood pressure, chronic heart or lung disease, or a history of stroke.
- Physical Features: A small jaw or a large neck circumference.
Diagnosis
Diagnosing sleep apnea typically involves a sleep study. There are two main types:
- Polysomnography (In-Lab Sleep Study): This is a comprehensive test usually conducted in a hospital or sleep center. It monitors many body functions during sleep, including brain waves, eye movements, muscle activity (to analyze sleep stages), heart rate, breathing patterns, oxygen levels, snoring intensity, and sleep positions.
- Home Sleep Apnea Test (Portable): This is a simpler test that can be done at home. The portable device is lightweight and mainly records your breathing patterns, heart rate, and oxygen levels.
If you suspect you have sleep apnea, the first step is to consult a doctor. They will evaluate your symptoms and risk factors to determine if a sleep study is needed and which type is most appropriate for you.
Treatment and Management
Managing sleep apnea often involves a combination of lifestyle changes and medical treatments.
A. Healthy Lifestyle Habits
Weight Management: Maintaining a healthy weight through a balanced diet and regular exercise is often the first and most important step.
Sleeping Position: Some people have more severe apnea when sleeping on their back. Sleeping on your side can help keep the airway open.
Manage Nasal Congestion: Controlling allergies or a stuffy nose can improve airflow through the nasal passages.
Avoid Triggers: Smoking causes swelling in the airway lining. Alcohol, sleeping pills, and sedatives relax the throat muscles, worsening apnea. Quitting smoking and avoiding alcohol and sedatives before bed are crucial preventive measures.
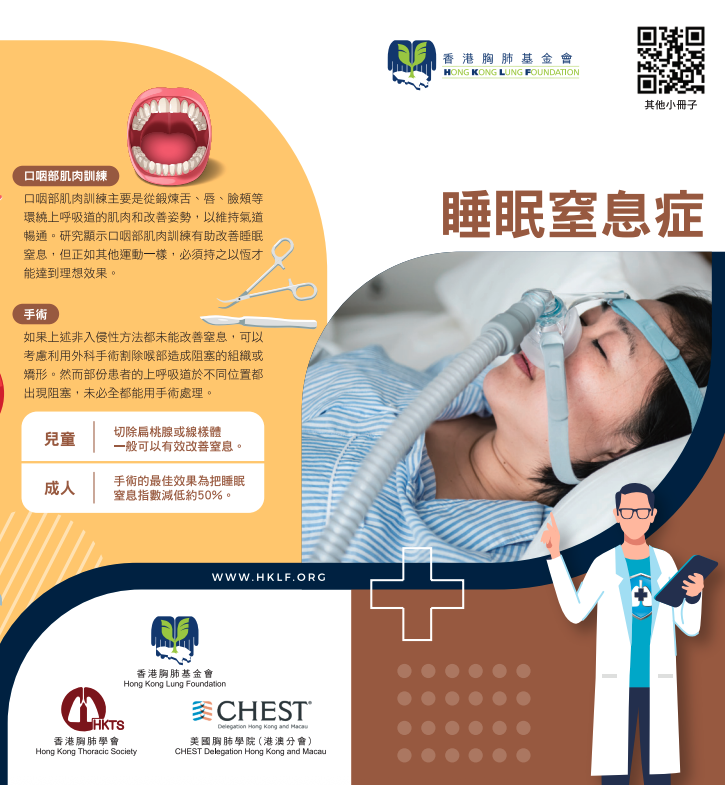
B. Continuous Positive Airway Pressure (CPAP) Therapy
CPAP therapy is the most safe and effective treatment for sleep apnea.
How it works: A machine delivers a continuous, gentle stream of pressurized air through a mask (covering the nose or nose and mouth). This air pressure acts as a splint, keeping the airway open during sleep.
Types: CPAP machines can deliver a fixed pressure or automatically adjust the pressure based on your breathing needs throughout the night.
Adapting to Therapy: It can take time to get used to sleeping with the mask. Using a heated humidifier can help alleviate dryness in the nose or throat and improve comfort. While CPAP does not cure sleep apnea, it is a highly effective way to control the condition and must be used regularly to experience benefits.
C. Oral Appliance (Dental Device)
How it works: A custom-fitted device, similar to a mouthguard, is made by a dentist. The patient wears it during sleep to hold the jaw forward, which helps prevent the tongue from collapsing backward and blocking the airway.
Considerations: This treatment is effective for some patients, particularly those with mild to moderate OSA. A follow-up sleep study is often recommended to confirm the device is working. Potential side effects can include discomfort in the jaw joint or teeth.
D. Surgery
How it works: If non-invasive treatments are unsuccessful or unsuitable, surgery may be considered to remove or reduce excess tissue blocking the airway or to correct structural abnormalities. Hypoglossal nerve stimulation has also been introduced in recent years.
Considerations: Surgery is not an option for everyone, as blockages can occur at multiple levels in the airway. Its effectiveness varies from person to person, and there is a risk of the condition recurring over time.
Orofacial Myofunctional Therapy
Orofacial myofunctional therapy may be used as an adjunctive treatment in selected patients with obstructive sleep apnoea. It involves exercises that strengthen the muscles of the tongue, mouth and throat, which may help improve upper airway stability during sleep.
Last updated: March 2026

