Chronic Obstructive Pulmonary Disease (COPD)
Overview
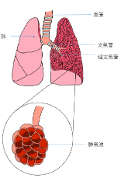
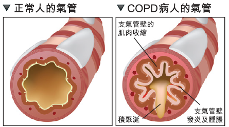
Chronic obstructive pulmonary disease (COPD) is a long-term condition affecting the lungs, which causes difficulty breathing because the airways are narrowed, and tissues inside the lungs are damaged. Most patients experience worsening over time, but proper treatment and changes to lifestyles can help to improve symptoms and quality of life.
COPD includes subtypes of disease such as chronic bronchitis (long-lasting cough with mucus/sputum production) and emphysema (damaged air sacs within the lungs which can be abnormally enlarged, leading to shortness of breath). Many patients with COPD have one or both conditions.

Common Symptoms
COPD often has a slow onset, and symptoms may be difficult to detect at first. Over time, symptoms can become more noticeable. Common symptoms may include:
- Shortness of breath, particularly on exertion or exercise
- Chronic cough lasting months to years
- Excessive mucus production, with phlegm with most coughs
- Wheezy breathing
- Chest tightness
- Becoming easily tired
- Frequent chest infections
Causes / Risk Factors
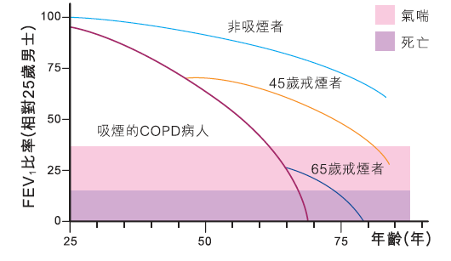
COPD in many patients is caused by airway and lung damage by exposure to harmful substances. Common causes and risk factors include:
- Cigarette smoke, including active smoking and second-hand smoke
- Air pollution from factories, chemical plants, or other environmental sources
- Indoor exposure such as cooking indoors without adequate ventilation
- Genetic risk factors, which may make certain patients more likely to develop COPD
Diagnosis
Diagnosis of COPD requires a combination of history taking, physical examination, and more specific investigations. Common assessments include:
- History taking, including symptoms, smoking exposure, occupational exposure, and past medical history
- Physical examination, including listening to the chest and examining oxygen levels
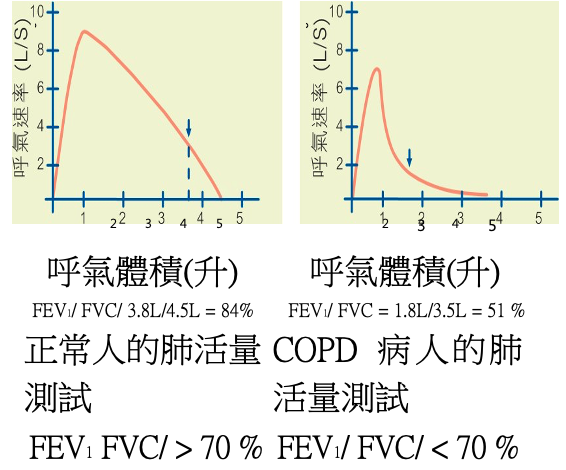
- Spirometry or lung function testing for airway function assessment
- Further tests in selected patients, such as chest X-rays, CT scan of the lungs, or blood tests
(圖三)
Treatment and Management
Treatment can involve both drug and non-drug treatments. The goals are to reduce symptoms, prevent acute flare-ups, improve activity tolerance, and maintain quality of life.
Drug treatment may include:
- Inhaled bronchodilators, which help to open up the airway by relaxing the airway muscles
- Inhaled steroids, which help to reduce swelling and inflammation in the airways. Steroids help to reduce acute episodes of illness but can also increase the risk of pneumonia
- Oral phosphodiesterase 4 inhibitors, which help to reduce acute flares in selected patients
- Antibiotics and oral steroids used during acute flares
- Mucus-clearing agents, which are usually taken orally
Non-drug treatment may include:
- Stopping smoking to prevent ongoing damage to the airways and lungs
- Pulmonary rehabilitation, which consists of a supervised exercise program involving specific exercises and breathing techniques
- Regular exercise
- Vaccinations to prevent serious infections
- Healthy diet and weight management
- Consideration of surgical treatments in selected patients with severe illness to improve their quality of life
Living with COPD
COPD is a chronic condition, but patients can still live fruitful lives with a good degree of quality with proper treatment and assistance. Helpful measures include:
- Attend medical follow-ups on time
- Avoid smoking
- Stay physically active
- Maintain good personal hygiene
- Have a backup plan for any acute flare-ups
- Join support groups for patients with similar problems
When to Seek Medical Attention
It is important to seek emergency medical attention if any of the following occur:
- Symptoms are worsening
- It is becoming hard to cope with daily life
- Severe shortness of breath
- Confusion
- Very rapid heartbeat
Conclusion
COPD can be well managed with proper treatment including medicine and lifestyle changes. Stopping smoking is of utmost importance to prevent the disease from worsening. Inhaled medications are the cornerstone of treatment. Staying active and engaging in rehabilitation and regular exercise help to maintain quality of life. Vaccinations help to prevent complications and hospitalizations. Working with healthcare providers helps ensure the best outcomes.
Last updated: March 2026






