Pneumonia
Overview
Pneumonia is an inflammation of lung tissue that is usually caused by infection with bacteria or viruses. It can cause mild to life-threatening illness in people of all ages. In 2023, it was the second leading cause of death in Hong Kong.
Types of Pneumonia
- Community-acquired pneumonia (CAP): It is the most common type which refers to pneumonia acquired outside of a medical or institutional setting.
- Hospital-acquired pneumonia (HAP):. It refers to pneumonia acquired during a hospital stay. It can be more serious than other types as it may involve drug-resistant bacteria or patients with weaker immunity due to other illnesses.
- Aspiration pneumonia: It is due to the inhalation of foreign material, like food, saliva and vomitus, into the airways. This is often due to dysphagia, reduced consciousness or neurological disorders.
- Ventilator-associated pneumonia (VAP): It refers to pneumonia acquired when a patient is in ventilated condition.

Causes/ risk factors
Some people are at higher risk for severe pneumonia:
- Young children and infants
- Older adults (65 years old or above)
- People with weakened immune systems (for example, HIV carrier, on chemotherapy or immunosuppressive drug)
- Those with chronic illness (for example, heart disease, diabetes, lung disease and kidney disease)
- Chronic smoker or drinker
- Those after surgery or critical illness and those on ventilator for breathing
Common Symptoms
- Shortness of breath
- Coughing
- Fever and chills
- Chest pain that worsens when breathing deeply
- Fatigue and weakness
- Sputum production
- Upper respiratory traction infection symptoms (e.g. runny nose, sore throat, headache, and muscle aches)
Diagnosis
History taking and physical examination
Sputum culture: helps identify bacterial infection and guide antibiotic treatment.
Upper respiratory tract samples: help identify viral infection; in selected situations, other microbiological tests may help identify the causative organism.
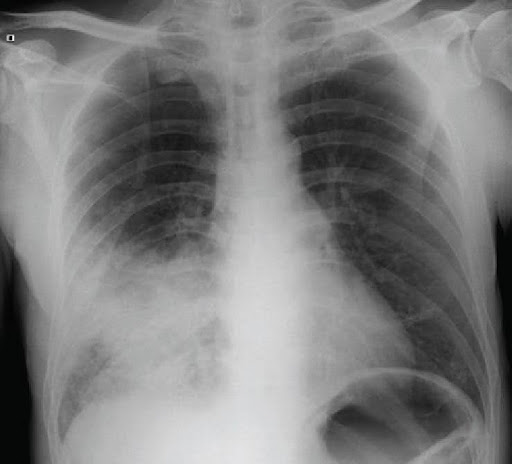
Chest X-ray: helps assess the presence, location and extent of lung inflammation.
Blood tests: white cell count and other tests may help assess infection severity, overall condition and possible complications.
Complications
Respiratory failure: may lead to low oxygen level or carbon dioxide retention and may require ventilatory support.
Fluid and pus accumulation: may refer to pleural effusion or a pus-filled cavity in the lung tissue.
Sepsis and organ damage: severe infection and inflammation may lead to organ failure and, in some cases, disseminated intravascular coagulation (DIC).
Treatment and Management
- Bacterial pneumonia: treated with antibiotics.
- Viral pneumonia: may require antiviral treatment in selected cases.
- Supportive care: rest, adequate fluids and fever-reducing medications.
It is important to follow your doctor’s instructions and complete the full course of medication. Some patients may require hospital admission if the condition is serious.
Prevention
- Practice good hand hygiene.
- Get vaccinated, such as pneumococcal, influenza, COVID-19 and respiratory syncytial virus (RSV) vaccines. It is advisable to discuss with your doctor which vaccines are suitable for you.
- Avoid smoking and exposure to smoke.
- Maintain a healthy immune system through proper nutrition and rest.
- Practice respiratory etiquette, such as covering coughs and sneezes.
- Take precautions when in contact with potentially infected animals and avoid travel to outbreak areas where appropriate.
Last updated: March 2026